Treatment Options
Fortunately, there are many treatments for conditions
affecting the liver and its related biliary system.
Liver transplantation is the procedure of last resort
for people with severe liver disease and liver failure.
Although cirrhosis is the leading cause of liver failure,
every patient with cirrhosis does not require a liver
transplant. This is because of the large size of the
liver and the ability of the liver to regenerate itself
until the last stages.
Liver Cancer
(Hepatoma)
There are numerous factors a liver specialist takes
into account when recommending treatment for a person
with liver cancer, including the stage of the cancer;
the condition of the liver; and the size and location
of the tumors. Not every treatment described below is
the best choice for every patient.
Liver Resection
Resection is the surgical removal of a tumor and surrounding tissue. A partial hepatectomy or liver resection is the removal of the tumor-containing portion of the liver, varying from a wedge (like a slice of pie) or an entire lobe. In time, the remaining liver regenerates. Resection can be performed alone or in combination with other treatments, such as radiofrequency ablation or microwave coagulation therapy, which uses high temperatures to destroy the tumor. The main obstacle to performing a resection for a liver cancer is the presence of cirrhosis, which limits the ability of the liver to regenerate. This limits the surgeon from treating many patients who could otherwise benefit from a liver resection because of the high likelihood of liver failure developing after the surgery. When resections are performed, patients are expected to be in the hospital for 5-10 days.
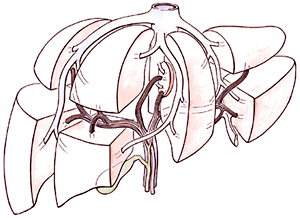 |
| Sections of the liver and their blood supply. |
Liver Transplantation
Liver transplantation is a suitable option for some patients with liver cancer, especially those with early stage tumors that would have been removable by resection had it not been for the cirrhosis. When liver transplantation is performed in appropriate candidates with hepatoma, approximately 85% are cured of the liver cancer.
Radiofrequency Ablation or RFA
During this non-invasive procedure, a special needle is guided through the skin into the tumor using imaging and placed within the lesion. Then, radiofrequency current is delivered to the tumor site. The intense heat “cooks” the tumor just as food is cooked in a microwave oven. Radiofrequency ablation works best on smaller tumors (2-3 cm in diameter) and tumors that are located deep in the liver and away from major blood vessels. However, there is no guarantee that the cancer will not come back. To minimize the discomfort during the procedure, RFA is done under general anesthesia and patients may stay overnight in the hospital.
 |
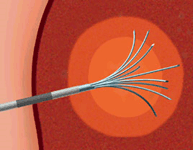 |
A needle is placed through the skin directly into the liver tumor, and a bouquet of very thin electrodes is then extended from the end of the needle into different portions of the tumor. This will allow heating of the entire tumor. |
By the end of the ablation procedure the tumor has been heated to a temperature sufficient to cause death of the tumor cells. |
Microwave Coagulation Therapy (MCT)
Similar to RFA, MCT is usually performed under ultrasound or CT guidance. Once the needle is in the tumor, MCT is used to burn and kill the tumor. Microwave ablation burns better and faster and is used for larger tumors. This technique may be used to downstage the tumor to meet transplant guidelines, making the patient eligible for liver transplant.
Chemoembolization
 |
|
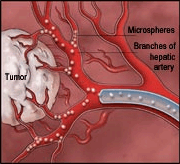
In this minimally invasive technique, resembling a cardiac catheterization procedure, chemotherapeutic agents are delivered directly to the artery in the liver that feeds the tumor. Not only is chemotherapy sent right to the place it is needed, the artery feeding the tumor is also blocked, limiting blood flow to the tumor and choking it by depriving the tumor cells of oxygen. Unlike traditional chemotherapy given through an IV in the arm, chemoembolization rarely causes the generalized side effects known to be associated with chemotherapy such as nausea, vomiting, hair loss, etc. While chemoembolization is not a cure for liver cancer, it can keep tumors from growing and prolongs life span considerably. Chemoembolization is most often done under intravenous sedation and sometimes patients stay overnight for observation.
Alcohol Injection
Ironically, while excessive alcohol use may cause liver cirrhosis, it can kill cancerous tumors when it is injected into the liver tumor. Similar to RFA (see above) it is most successful in smaller sized tumors. Alcohol is injected through a thin needle passed through the skin and positioned into the tumor. Because of the pain caused by alcohol’s effect on tissues, this procedure is done under either heavy sedation or general anesthesia.
Chemotherapy
Systemic chemotherapy (that which travels through the bloodstream) does not cure liver cancer, but it can reduce the size of a tumor and also relieve pain. However, the medications currently available for treating liver cancer are not as effective as medications available to treat other common cancers such as breast, colon and prostate.
Chemotherapy is often used in conjunction with other treatments and after other treatment options have been exhausted.
Radiation
Liver cancer is generally not responsive to radiation therapy, but similar to chemotherapy, it can shrink the tumor and relieve pain.
Biliary Disorders
The bile ducts can be prone to blockage by stones, narrowing, or tumors. Opening up blocked ducts and removal of the blockage restores the flow of bile and relieves pain and/or jaundice.
Bile Duct Cancer (Cholangiocarcinoma)
 |
|
Usually, a bile duct that contains a malignant tumor is resected, or removed. Unlike simple removal of the gallbladder, which is most often done via a laparoscope (minimally invasive surgery), the removal or resection of a bile duct tumor (which can also include removing parts of the gall bladder, liver, pancreas or small intestine) is done through an “open approach” or a large incision. If the tumors cannot be removed completely, there are procedures that can unblock the obstructions, which provide considerable relief and prolongation of life span. When surgery is not possible, radiation either alone or with chemotherapy is a course of treatment.
Bile Duct Strictures
When bile ducts - the tiny, quill like passageways through which bile drains - are irritated (from inflammation) or injured, they become narrow. This abnormal narrowness is called a stricture. Strictures can be caused by cancer or by unintentional injury to the ducts during certain laparoscopic procedures (particularly removal of the gall bladder). Bile duct repair involves surgery that can be relatively simple or complex; if infection has occurred, that must be treated, also. One method, the Roux-en-Y hepaticojejunostomy, restores bile flow by connecting bile ducts to the small intestine for adequate drainage. The earlier a bile duct injury is detected and repaired, the better. Over time, an untreated and blocked bile duct will lead to a build-up of bile in the liver and causes cirrhosis.
Pancreatic Cancer
 |
|
In the "Standard Whipple Procedure," part of the stomach is also removed while, in the "Pylorus-Preserving Whipple Procedure," the entire stomach is retained. After completing the resection, the surgeon reconnects the intestine to the bile duct, pancreas, and stomach so that the patient can eat normally. |
|
Very few patients with pancreatic cancer are candidates for surgery and instead receive radiation and chemotherapy, the latter particularly to relieve pain. For those who are, the procedure that is performed depends partly on the tumor’s location.
When the tumor is located at the head of the pancreas (as is most often the case), a complex surgery known as the Whipple procedure is performed, which involves removal of not only part of the pancreas, but also the duodenum, the gallbladder, a segment of the bile duct, and sometimes part of the stomach. Bile flow is reestablished by connecting the bile duct and the rest of the pancreas to the small intestine. If the cancer is in the mid-section or tail of the pancreas, a distal pancreatectomy is performed to remove the cancer.
Pancreatic cancer can be very painful, so while there might not be a cure in sight for the patient, physicians, including those at University Hospital, do their best to keep patients comfortable. For example, the bile ducts of patients with pancreatic cancer can become blocked, leading to jaundice and related lack of appetite and itching. By stent placement, gastroenterologists can open the blocked bile ducts and relieve the symptoms of jaundice. To ease the pain of pancreatic cancer, a celiac nerve block can be used to inject certain agents, such as alcohol or a steroid, into the identified nerve or nerves. The numbness brings pain relief that medications cannot match.
Hepatitis C
Deciding which medications to use is based on several factors, including the existence of cirrhosis, co-morbidities, hepatitis C genotype, current viral load and the patient's response to previous treatment.